Abstract
Background: Living in low-income neighbourhoods and being an immigrant are each independently associated with adverse neonatal outcomes, but it is unknown if disparities exist in the neonatal period for children of immigrant and nonimmigrant females living in low-income areas. We sought to compare the risk of severe neonatal morbidity and mortality (SNMM) between newborns of immigrant and nonimmigrant mothers who resided in low-income neighbourhoods.
Methods: This population-based cohort study used administrative data for females residing in low-income urban neighbourhoods in Ontario, who had an in-hospital, singleton live birth at 20–42 weeks’ gestation, from 2002 to 2019. We defined immigrant status as nonrefugee immigrant or nonimmigrant, further detailed by country of birth and duration of residence in Ontario. The primary outcome was a SNMM composite (with 16 diagnoses, including neonatal death and 7 neonatal procedures as indicators), arising within 0–27 days after birth. We estimated relative risks (RRs) and 95% confidence intervals (CIs) using modified Poisson regression with generalized estimating equations.
Results: Our cohort included 148 050 and 266 191 live births among immigrant and nonimmigrant mothers, respectively. Compared with newborns of non-immigrant females, SNMM was less frequent among newborns of immigrant females (49.7 v. 65.6 per 1000 live births), with an adjusted RR of 0.76 (95% CI 0.74 to 0.79). The most frequent SNMM indicator was receipt of ventilatory support. Relative to neonates of nonimmigrant females, the risk of SNMM was highest among those of immigrants from Jamaica (adjusted RR 1.14, 95% CI 1.05 to 1.23) and Ghana (adjusted RR 1.20, 95% CI 1.05 to 1.38), and lowest among those of immigrants from China (adjusted RR 0.44, 95% CI 0.40 to 0.48). Among immigrants, the risk of SNMM declined with shorter duration of residence before the index birth.
Interpretation: Within low-income urban areas, newborns of immigrant females had an overall lower risk of SNMM than those of nonimmigrant females, with considerable variation by maternal birthplace and duration of residence. Initiatives should focus on improving preconception health and perinatal care within subgroups of females residing in low-income neighbourhoods.
Neonatal morbidity and mortality are important public health indicators used to monitor and evaluate neonatal health and quality of perinatal care.1,2 The neonatal period, ranging from birth to 27 days thereafter, is the most vulnerable time for infant survival.1 Around 75% of infant deaths occur during this period, largely from prematurity and other conditions that can often be prevented by timely obstetrical and neonatal care.3,4
In high-income countries, improvements in health care have resulted in a decline in neonatal mortality,5,6 including in Canada, where the rate is 3.6 deaths per 1000 live births.7 Accordingly, research and public health surveillance has increasingly focused on severe neonatal morbidity (SNM), which refers to a newborn who has survived a severe complication during birth or the neonatal period.1,8,9 Identifying newborns at high risk of SNM is crucial as it has serious implications for the surviving child and their family.10,11
Limited research has examined SNM in high-income countries.2,6,8,12–17 Studies have primarily focused on deriving and validating the criteria to define SNM,1,3,10 quantifying the prevalence of SNM and identifying risk factors in African, Asian and Latin American regions.11,18–27 Research is also lacking on a range of upstream social determinants of health inequity and their influence on SNM.28,29 Living in a low-income area12,30–35 and being an immigrant36–46 are each independently associated with adverse neonatal outcomes. However, studies about area-level income have only made comparisons across income groups (e.g., females living in low-v. high-income areas), rather than being confined to low-income areas, where the risk of adverse neonatal outcomes may be highest and where enhanced obstetric and neonatal care are most needed. Thus, these studies may not have effectively disentangled the influence of area-level income from that of being a new immigrant who may settle in a low-income area or a nonimmigrant female living in a low-income area.
This study builds on our previous work, in which we found that females residing in the lowest-income areas were at highest risk of having a newborn with concomitant preterm birth and severe small-for-gestational-age birth weight.35 Furthermore, immigrant females had a slightly lower overall risk of severe maternal morbidity or mortality (SMMM) than nonimmigrant females, all of whom were residing within low-income areas.47
In this study, we sought to compare the risk of SNMM between newborns of immigrant and nonimmigrant females residing in low-income urban neighbourhoods. We further sought to evaluate risk of SNMM by maternal world region of birth and country of birth, and by duration of residence among immigrant females.
Methods
Study design and setting
We conducted this retrospective, population-based cohort study in Ontario, the most populous and ethnically diverse province in Canada. Ontario receives about 53% of all female immigrants entering Canada,48 many of whom originate from nations where rates of SNMM are relatively high,10 and many reside in low-income urban areas upon arrival.48 We report our findings according to the Reporting of Studies Conducted using Observational Routinely Collected Data (RECORD) checklist.49
Participants
We included all in-hospital, singleton live births at 20–42 weeks’ gestation, from 2002 to 2019. We limited the cohort to births to females aged 15–50 years who had a valid Ontario Health Insurance Plan (OHIP) number and who resided in urban neighbourhoods of the lowest income quintile as of the index birth date (Appendix 1, Table S1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221711/tab-related-content).
Data sources
We used administrative data at ICES, an independent, nonprofit research institute whose legal status under Ontario’s health information privacy law allows it to collect and analyze health care and demographic data, without consent, for health system evaluation and improvement. Data sets used for this study are valid and reliable sources for perinatal research, described in Appendix 1, Table S2.50–54 These deidentified data sets are linked using unique encoded identifiers and analyzed at ICES.
All live births were identified in the MOMBABY database, which captures labour and delivery records for about 98% of Ontario births.50–52 Maternal immigrant status was determined using the Immigration, Refugees and Citizenship Canada Permanent Residents database (Appendix 1, Table S2).53,54 Neighbourhood income quintile was categorized using Statistics Canada’s Postal Code Conversion File Plus (PCCF+, version 7B), based on the female’s residential postal code at the time of the index birth.55
Exposures
The primary exposure was maternal immigrant status before the index birth, defined according to a female’s birthplace and migration status. Henceforth, we refer to nonrefugee immigrants as “immigrants,” and females born in Canada as “nonimmigrants.” We excluded refugees or other special-status immigrants, and females concomitantly classified as both a nonimmigrant and immigrant. We also omitted immigrants who did not have a landing date, or those whose landing date either preceded their own date of birth or was after the index delivery date (Appendix 1, Table S1).
We defined 3 secondary exposures, namely world region of birth, country of birth and, for immigrant females, duration of residence in Ontario. We categorized world region of birth according to a modified version of the United Nations classification scheme (i.e., Canada, Caribbean, East Asia and Pacific, Latin America, Middle East and North Africa, South Asia, Sub-Saharan Africa, and Western Nations and Europe).56–58 We identified country of birth for those who had immigrated from the 20 countries contributing the greatest number of births in Ontario during the study period. For immigrant females, we calculated duration of residence as a continuous variable, defined by the number of years between their landing date in Ontario and the index birth date.
Outcomes
The primary outcome was a composite of SNM and all-cause neonatal mortality (SNMM). We measured SNMM in our study using the English-version Neonatal Adverse Outcomes Indicator (E-NAOI), defined as the presence of 1 or more E-NAOI components arising in the index birth admission and up to 27 days there-after.8 The E-NAOI consists of 16 neonatal diagnoses (including neonatal death) and 7 procedures that relate to different body systems.8 The components are equally weighted. They are recorded using diagnostic codes (e.g., seizures) from the Canadian version of the International Classification of Diseases and Related Health Problems, 10th Revision (ICD-10-CA) and procedural codes (e.g., resuscitation, ventilatory support) from the Canadian Classification of Health Interventions (Appendix 1, Table S1).8 The E-NAOI has shown good concurrent validity as a population measure of SNM, and predictive validity for infant death and hospital readmission in the first year of life.8
A secondary outcome was the number of SNMM indicators (i.e., E-NAOI components) that were present at the index birth admission and up to 27 days thereafter, categorized as 0 (referent), 1, 2 or 3 or more indicators.59 For this secondary outcome, neonatal death and neonatal diagnoses or procedures were not mutually exclusive categories (e.g., we classified a newborn who died after having a seizure as having an SNMM score of 2).
Statistical analysis
Given ICES privacy and security requirements, ICES staff (A.B. and J.G.) generated the study cohort. One author (J.A.J.) completed the analyses using SAS version 9.4 (SAS Institute).
We compared means and proportions between immigrant and nonimmigrant females and their newborns for birth characteristics using standard differences, with a value greater than 0.10 considered to be a clinically meaningful difference.60
We used modified Poisson regression with generalized estimating equations (GEEs) to estimate relative risks (RRs), absolute risk differences and 95% confidence intervals (CIs) for the main outcome of SNMM (i.e., the presence of ≥ 1 E-NAOI components v. none), comparing newborns of immigrant and nonimmigrant females.61–63 We used this modelling approach to analyze the risk of SNMM for maternal world region of birth and country of birth, with females born in Canada as the referent. Generalized estimating equations, with an exchangeable correlation structure, accounted for correlation among females who had more than 1 live birth during the study period.64 We adjusted RRs and absolute risk differences for maternal age (15–19 yr, 20–29 yr, 30–39 yr, 40–50 yr),21,24 parity (0, 1, 2, ≥ 3)65 and any newborn structural congenital anomaly (yes or no),1 each determined in the index birth admission.
For the outcome of the number of SNMM indicators, we calculated odds ratios (ORs) using multinomial logistic regression with a robust error variance and GEE, comparing newborns of immigrant and nonimmigrant females. We adjusted ORs for the same variables as the main analysis.
In an immigrant-only analysis, after conducting multivariable fractional polynomial regression,66 we observed a nonlinear (quadratic) relation between maternal duration of residence and the risk of SNMM. Accordingly, we used a modified Poisson regression GEE model with a restricted cubic spline function to estimate adjusted RRs and 95% CIs of SNMM by declining duration of residence, compared with residing in Ontario 20 years or longer before the index birth.67 We adjusted RRs for the same variables as the main analysis, as well as world region of birth16 and other variables documented at arrival to Canada, including immigration class (economic, sponsored family),46 highest level of education (secondary school or less; trade certificate or diploma, or some university; university degree; graduate degree)27 and self-reported English and/or French language ability (yes or no).16,68
For the first sensitivity analysis, we removed gestational age at birth less than 32 weeks and a birth weight less than 1500 g from the SNMM composite for the main model, as neither are disease states, per se. The second analysis stratified the previous model by gestational age (births occurring < 32 or ≥ 32 weeks’ gestation), since birth before 32 weeks’ gestation is a major contributor to morbidity and mortality.5,69 The third analysis expanded the cohort to live births and stillbirths born at 20 weeks’ gestation or later, and compared SNM or perinatal mortality in the index birth admission and up to 27 days thereafter for newborns of immigrant and nonimmigrant females.
Ethics approval
Ethics approval was received from the University of Toronto Research Ethics Board (no. 00040721).
Results
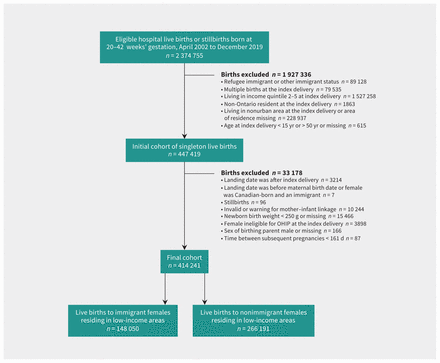
Of the 2 374 755 births during the study period, 414 241 were singleton live births to 312 124 females residing in a lowest-income (quintile 1) urban neighbourhood at the time of the index birth (Figure 1). Among these live births, 148 050 were to immigrant females and 266 191 were to nonimmigrant females (Table 1).
Flow diagram of cohort creation. Note: OHIP = Ontario Health Insurance Plan.
Characteristics of births among immigrant and nonimmigrant females residing in a low-income urban neighbourhood*
Immigrant females were older than nonimmigrant females (30.6 yr v. 27.9 yr) and more likely to be parous, and their newborns had a lower mean birthweight (Table 1). Mean gestational age at birth, and proportions of preterm births and structural congenital anomalies, did not differ appreciably (Table 1).
Most immigrants had originated from South Asia (n = 52 428, 35.4%) and the East Asia and Pacific region (n = 35 276, 23.8%); 111 626 (75.4%) immigrants had resided in Ontario for less than 10 years (Table 1). Additional characteristics are presented in Table 1.
Indicators of SNMM
The 5 most frequent SNMM indicators were the same among newborns of immigrant and nonimmigrant females. These were ventilatory support, receipt of intravenous fluids, gestational age at birth of less than 32 weeks, birth weight of less than 1500 g and respiratory distress syndrome (Appendix 1, Table S3).
Immigrant status and SNMM
The rate of SNMM (the presence of ≥ 1 E-NAOI components v. none) was significantly lower among newborns of immigrant (49.7 per 1000 live births) than nonimmigrant (65.6 per 1000 live births) females, equivalent to an adjusted RR of 0.76 (95% CI 0.74 to 0.79) and an adjusted absolute risk difference of −15.2 cases per 1000 live births (95% CI −16.6 to −13.8) (Table 2).
Risk of severe neonatal morbidity and neonatal mortality (SNMM) arising in the index birth admission and up to 27 days thereafter, comparing newborns born to immigrant and nonimmigrant females*
Compared with their nonimmigrant counterparts, the newborns of immigrant females had lower odds of having 1 SNMM indicator (adjusted OR 0.74, 95% CI 0.71 to 0.76), 2 indicators (adjusted OR 0.68, 95% CI 0.64 to 0.73) and 3 or more indicators (adjusted OR 0.82, 95% CI 0.78 to 0.86) (Table 3).
Odds ratio of having a higher number of severe neonatal morbidity and neonatal mortality (SNMM) indicators versus having 0 SNMM indicators in the index birth admission and up to 27 days thereafter, comparing newborns born to immigrant and nonimmigrant females*,†,‡
Maternal birthplace and SNMM
Relative to newborns of nonimmigrants, the risk of SNMM was lower for newborns of immigrant females from South Asia (adjusted RR 0.72, 95% CI 0.69 to 0.75), Middle East and North Africa (adjusted RR 0.70, 95% CI 0.65 to 0.76), East Asia and Pacific (adjusted RR 0.67, 95% CI 0.64 to 0.71), Latin America (adjusted RR 0.79, 95% CI 0.73 to 0.87), and Western Nations and Europe (adjusted RR 0.77, 95% CI 0.71 to 0.83) (Table 4). Conversely, the risk was higher for those of immigrant females from the Caribbean (adjusted RR 1.12, 95% CI 1.04 to 1.19).
Risk of severe neonatal morbidity and neonatal mortality (SNMM) arising in the index birth admission and up to 27 days thereafter, comparing newborns of immigrants from each world region of origin and those of nonimmigrant females*
Newborns of females from Jamaica (adjusted RR 1.14, 95% CI 1.05 to 1.23) and Ghana (adjusted RR 1.20, 95% CI 1.05 to 1.38) had the highest risk of SNMM relative to their nonimmigrant counterparts, when data relating to the top 20 immigrant countries contributing to births were analyzed, while the lowest risk was among newborns of females from China (adjusted RR 0.44, 95% CI 0.40 to 0.48) (Table 5).
Risk of severe neonatal morbidity and neonatal mortality (SNMM) arising in the index birth admission and up to 27 days thereafter, among newborns of immigrant mothers from the 20 countries contributing the greatest number of births in Ontario, relative to newborns of nonimmigrant females*
Maternal duration of residence and SNMM
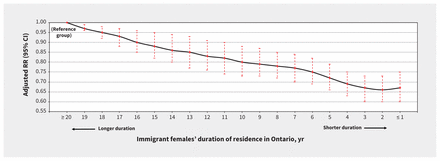
The risk of SNMM declined among newborns of immigrants with shorter duration of residence in Ontario, relative to newborns of immigrants who had resided in Ontario for 20 years or more (Figure 2).
Adjusted relative risk (RR) of severe neonatal morbidity and neonatal mortality (SNMM) arising in the index birth admission and up to 27 days thereafter by declining duration of residence in Ontario. Those residing in Ontario for at least 20 years are the reference group. Data are restricted to immigrant females residing in urban neighbourhoods of the lowest income quintile, and who had a singleton, in-hospital live birth at 20–42 weeks’ gestation in Ontario, Canada, from 2002 to 2019. Analysis adjusted for maternal age (15–19 yr, 20–29 yr, 30–39 yr, 40–50 yr), parity (0, 1, 2, ≥ 3), any structural congenital anomaly (yes or no), world region of birth (Caribbean, East Asia and Pacific, Latin America, Middle East and North Africa, South Asia, SubSaharan Africa, Western Nations and Europe), and the following variables at arrival to Canada: highest level of education (secondary school or less; trade certificate or diploma, or some university; university degree; graduate degree), English and/or French language ability (yes or no) and immigration class (economic, sponsored family). Analysis excludes 266 191 nonimmigrant females, 505 immigrant females missing highest level of education at arrival to Canada, 38 females missing world region of birth and 18 immigrant females missing English and/or French language ability at arrival to Canada. Note: CI = confidence interval.
Sensitivity analyses
After removing the 2 nondiagnostic indicators (gestational age at birth < 32 weeks and birthweight < 1500 g) from the SNMM composite, the risk estimates were largely unchanged (Appendix 1, Table S4). Rates of SNMM were higher among newborns delivered before 32 weeks’ gestation versus those born at or after 32 weeks’ gestation (Appendix 1, Table S5). Within both gestational age strata, newborns of immigrant females had a lower risk of SNMM than those of nonimmigrant females, especially those born at or after 32 weeks’ gestation (Appendix 1, Table S5). Inclusion of stillbirths and live births within the cohort did not materially change the risk estimates (Appendix 1, Table S6).
Interpretation
In this cohort of publicly insured females residing in low-income urban neighbourhoods in Ontario, newborns of immigrant females had an overall substantially lower risk of SNMM than newborns of nonimmigrant females. However, this association varied by maternal birthplace and duration of residence in Ontario. The risk of SNMM was higher among newborns of immigrants from the Caribbean world region; at a country level, those from Jamaica and Ghana; and those with a longer duration of residence in Ontario.
Our findings suggest that within low-income areas, newborns of immigrant females appear to have better neonatal outcomes than newborns of nonimmigrant females. This may be partly explained by the Healthy Immigrant Effect, which wanes with increasing duration of residency,70,71 as described by the Convergence Hypothesis.71 In addition, the Immigrant Paradox describes better health outcomes among immigrants than the native population within the host country, despite immigrants facing greater barriers to health care access.43,71,72
Our findings also suggest that the Healthy Immigrant Effect may transfer from a recent immigrant female to her newborn, as evidenced by a lower risk of SNMM, with some variation by maternal country of origin. Immigrant females who are healthier and more resilient may be most capable of migration; the immigration policy of a host country may preferentially select healthy immigrants.71 Another explanation may be that some immigrants have greater net income, educational achievement and health literacy than the average for a low-income neighbourhood. In contrast, some nonimmigrants may experience multigenerational poverty. The observed relation between shorter maternal duration of residence and lower SNMM may be owing to the movement of immigrant females whose newborns are at lowest risk of SNMM, out of low-income areas soon after their arrival to Ontario, while those who are similar to nonimmigrants remain in low-income neighbourhoods.
Previous studies have evaluated immigrant status6,16,17,46 or area-level income12,15 as independent risk factors for SNM, including some that used race and ethnicity as predictors of SNM.11,12 One Australian study found no association between immigrant status and SNM, but used an SNM composite with 3 indicators and no procedures.6 Previous Canadian research has yielded similar findings to our current study; however, the study cohorts in those and our current study overlap somewhat. One study used a composite outcome measure like ours, and observed a similar relation between immigrant status and SNM in Ontario.16 Other studies observed that the risk of adverse perinatal outcomes varied by maternal birthplace, including a higher risk among immigrant females from the Caribbean region, and countries such as Jamaica and Ghana, compared with Canadian-born females.44,45
The current study complements our previous research on neighbourhood income level and risk of concomitant preterm birth and small-for-gestational-age birth weight, by identifying attributes of mother–infant pairs who are at higher risk of adverse neonatal outcomes within lowest-income neighbourhoods.35 Collectively, the findings from this current study and recent data about SMMM among females residing in low-income neighbourhoods47 suggest that immigrant females and their newborns each have an overall lower risk of adverse birth outcomes than their Canadian-born counterparts.
This study highlights the importance of evaluating health outcomes like SNMM within area-level, constrained income groups, particularly when there is a known gradient effect across income levels. This approach can identify pregnant parents and newborns at highest risk, who stand to benefit the most from targeted screening, surveillance and services. Our findings also suggest that not all immigrants appear to experience the Healthy Immigrant Effect, which further emphasizes the importance of within-neighbourhood research to inform policy and practice regarding the needs of immigrants and their infants in low-income areas. The needs of nonimmigrants and their infants within low-income areas may not be uniform, and future studies should evaluate the multi-generational attributes of nonimmigrant populations. Furthermore, our findings underscore a need to move beyond using a dichotomous approach to immigrant status (i.e., immigrant v. non-immigrant) in policy, practice and research. Such aggregation bias, where distinct but smaller subgroups are categorized together, masks important nuances among immigrant subgroups.73
Limitations
We excluded multifetal pregnancies from the cohort, and findings may not be applicable to those newborns.74 A few stillbirths and neonatal deaths may have been missed within the data sets.75 Although the secondary outcome of the number of SNMM indicators has not been validated, it was akin to our approach in a previous study, where we observed that maternal mortality was exponentially associated with the number of severe maternal morbidity indicators.59
A small proportion of immigrant females may not have been linked to the Immigration, Refugees and Citizenship Canada Permanent Residents database and would have therefore been classified as nonimmigrants (i.e., Canadian-born). This may have occurred if their immigration record was missing or if they entered Ontario before 1985 or via another province. Such misclassification would tend to bias the results toward the null. We did not include refugees or other special-status immigrants in the study because they may have lacked an OHIP number for data linkage. Furthermore, as refugees tend to have different migration experiences (e.g., nonvoluntary migration and secondary migration) than non-refugee immigrants, our findings may not be generalizable to their newborns. Even so, newborns in both refugee and nonrefugee immigrant groups may experience similar degrees of SNMM.16
This study focused on newborns among females living in urban areas, so findings may not be generalizable to those living in low-income rural areas,76 given differences in health care access and health indicators between urban and rural residents.77 Neighbourhood income quintile reflects area-level income status;78 however, details of individual-level income were unavailable. A female lacking an up-to-date residential address may have been incorrectly assigned to the wrong neighbourhood income quintile, but the likelihood of this is low, given her active use of OHIP for antenatal and delivery care. Nonindependence may also have been present owing to clustering by geography (e.g., females in the same neighbourhood may be more similar than those in different neighbourhoods).
Data were not available on certain sociodemographic factors among nonimmigrants. Among immigrants, early life exposures and obstetrical events pre-migration were also unknown. In addition, we had no information on psychosocial, employment and behavioural factors (e.g., smoking, substance use), as well as measures of obesity and quality of care, potentially leading to residual confounding in all analytical models. Differences in SNMM between newborns of immigrant and nonimmigrant females, and by immigrant country of origin, may be explained by these factors. Future research is needed to clarify if the disparities we observed are owing to unmeasured confounders or true differences.
Conclusion
Among females residing in low-income urban areas in Ontario, newborns of immigrants had a considerably lower risk of SNMM than nonimmigrants. However, that risk varied by maternal birthplace and duration of residence in Ontario. Efforts should be aimed at improving the overall health and well-being of all females residing in low-income areas, and at determining if the risk of adverse birth outcomes can be equitably reduced among immigrant and non-immigrant groups. Research should also focus on females originating from specific countries and their newborns, who may require additional monitoring and interventions in the perinatal period.
Footnotes
Competing interests: Simone Vigod receives royalties from UpToDate for authorship of materials related to depression and pregnancy. She is the president of the Canadian Association of Psychiatric Epidemiology, and the president-elect of the Marce Society of North America (perinatal mental health). Patricia O’Campo reports funding from the Canadian Institutes for Health Research and the Public Health Agency of Canada, outside of the submitted work. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Jennifer Jairam, Patricia O’Campo and Joel Ray contributed to study concept and design. All of the authors acquired, analyzed or interpreted the data. Jennifer Jairam performed the statistical analysis. Jennifer Jairam, Patricia O’Campo and Joel Ray drafted the manuscript. All of the authors revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: Jennifer Jairam received PhD funding from University of Toronto Open Fellowship; University of Toronto, Dalla Lana School of Public Health, Doctoral Completion Award; University of Toronto School of Graduate Studies, Mary Gertrude I’Anson Scholarship; St. Michael’s Unity Health Toronto Research Training Centre Top-Up Award; Ontario Graduate Scholarship; and Queen Elizabeth II/C.P. Shah Graduate Scholarship in Science & Technology. The funding organizations had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Disclaimer: This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health (MOH) and the Ministry of Long-Term Care (MLTC). The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred. Parts of this material are based on data and/or information compiled and provided by the MOH, Canadian Institute for Health Information (CIHI), and Immigration, Refugees and Citizenship Canada Permanent Resident Database (IRCC-PRD) current to 2017. However, the analyses, conclusions, opinions and statements expressed in the material are those of the authors, and not necessarily those of MOH, CIHI or IRCC-PRD. Parts of this report are based on Ontario Registrar General (ORG) information on deaths, the original source of which is Service Ontario. The views expressed therein are those of the authors and do not necessarily reflect those of ORG or the Ministry of Public and Business Service Delivery. This document used data adapted from the Statistics Canada Postal Code Conversion File, which is based on data licensed from Canada Post Corporation, and/or data adapted from the Ontario Ministry of Health Postal Code Conversion File, which contains data copied under license from Canada Post Corporation and Statistics Canada.
Data sharing: The data set from this study is held securely in coded form at ICES. While data sharing agreements prohibit ICES from making the data set publicly available, access may be granted to those who meet pre-specified criteria for confidential access, available at https://www.ices.on.ca/DAS. The full data set creation plan and underlying analytic code are available from the authors upon request, understanding that the computer programs may rely upon coding templates or macros that are unique to ICES and are therefore either inaccessible or may require modification.
- Accepted April 17, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is non-commercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/